Ifuse Implant System
Sacroiliac Joint (SI Joint) Anatomy
The sacroiliac joint (SI joint) is located in the pelvis; it links the iliac bones (pelvis) to the sacrum (lowest part of the spine above the tailbone). It is an essential component for shock absorption to prevent impact forces from reaching the spine.
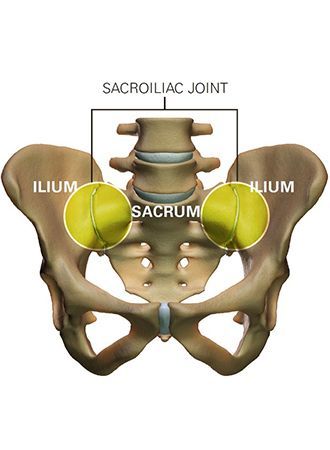
Do you have SI Joint Problems?
The SI joint is a significant cause of low back pain. Clinical publications have identified the SI joint as a pain generator in 15-30% of chronic low back pain patients (*1-4). In addition, the SI joint is a pain generator in up to 43% of patients with continued or new onset low back pain after a lumbar fusion (*5).
Like any other joint in the body, the SI joint can be injured and/or become degenerative. When this happens, people can feel pain in their buttock and sometimes in the low back and legs. This is especially true while lifting, running, walking or even sleeping on the involved side.
According to scientific data, it’s common for pain from the SI joint to feel like disc or low back pain. For this reason, SI joint disorders should always be considered in low back pain diagnosis.
Do you experience one or more of the symptoms listed below?
- Hip/groin pain
- Disturbed sleep patterns
- Feeling of leg instability (buckling, giving way)
- Sensation of low extremity: pain, numbness, tingling, weakness
- Low back pain
- Pelvis/buttock pain
- Pain going from sitting to standing.
- Disturbed sitting patterns (unable to sit for long periods, sitting on one side)
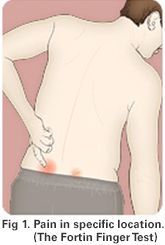


Making a Diagnosis
A variety of tests performed during physical examination may help reveal the SI joint as the cause of your symptoms. Sometimes, X-rays, CT-scan or MRI may be helpful in the diagnosis of SI joint-related problems.
The most relied upon method to accurately determine whether the SI joint is the cause of your low back pain symptoms is to inject the SI joint with a local anesthetic. The injection will be delivered under either X-ray or CT guidance to verify accurate placement of the needle in the SI joint. If your symptoms are decreased by at least 50%, it can be concluded that the SI joint is either the source of or a major contributor to your low back pain. If the level of pain does not change after SI joint injection, it is less likely that the SI joint is the cause of your low back pain.
iFuse Video Sacroiliac Joint Fusion
SI Joint Patient Video: Larry
Treatment Options
Once the SI joint is confirmed as the cause of your symptoms, treatment can begin. Some patients respond to physical therapy, use of oral medications, or injection therapy. These treatments are often performed repetitively, and frequently symptom improvement using these therapies is temporary. At this point, you and your surgeon may consider other options, including minimally invasive surgery.
TSI Joint Fusion with the iFuse Implant System®
The iFuse Implant System is designed to provide stabilization and fusion for certain SI joint disorders. This is accomplished by inserting triangular shaped titanium implants across the sacroiliac joint to maximize post surgical stability and weight bearing capacity.
The procedure is done through a small incision and takes about an hour.
Multiple published studies on iFuse have documented procedure safety and effectiveness (*6).
IMPORTANT: SI-BONE requests inclusion of the following indication and risk statement.
SI Joint Fusion with the iFuse Implant System®
The iFuse Implant System is designed to provide stabilization and fusion for certain SI joint disorders. This is accomplished by inserting triangular shaped titanium implants across the sacroiliac joint to maximize post surgical stability and weight bearing capacity. The procedure is done through a small incision and takes about an hour. Multiple published studies on iFuse have documented procedure safety and effectiveness.
References:
- Bernard TN, et al. Recognizing specific characteristics of nonspecific low back pain. Clin Orthop Relat Res. 1987;217:266–80.
- Schwarzer AC, et al. The Sacroiliac Joint in Chronic Low Back Pain. Spine. 1995;20:31–7.
- Maigne JY, et al. Results of Sacroiliac Joint Double Block and Value of Sacroiliac Pain Provocation Tests in 54 Patients with Low Back Pain. Spine. 1996;21:1889–92.
- Sembrano JN, et al. How Often is Low Back Pain Not Coming From The Back? Spine. 2009;34:E27–32.
- DePalma MJ, et al. Etiology of Chronic Low Back Pain Patients Having Undergone Lumbar Fusion. Pain Med. 2011;12:732-9.
- Polly, D.W.* et al., Neurosurgery. 2015. A list of additional published studies is available at www.si-bone.com/results
* Dr. Polly is an investigator on a clinical research study sponsored by SI-BONE. He has no financial interest in SI-BONE. Research was funded by SI-BONE, Inc.
SACROILIAC JOINT PAIN
OVERVIEW
Sacroiliac (SI) joint pain is felt in the low back and buttocks. The pain is caused by damage or injury to the joint between the spine and hip. Sacroiliac pain can mimic other conditions, such as a herniated disc or hip problem. Accurate diagnosis is important to determine the source of pain. Physical therapy, stretching exercises, pain medication, and joint injections are used first to manage the symptoms. Surgery to fuse the joint and stop painful motion may be recommended.
What is sacroiliac joint pain?
The SI joints are located between the iliac bones and the sacrum, connecting the spine to the hips. The two joints provide support and stability, and play a major role in absorbing impact when walking and lifting. From the back, the SI joints are located below the waist where two dimples are visible.
Strong ligaments and muscles support the SI joints. There is a very small amount of motion in the joint for normal body flexibility. As we age our bones become arthritic and ligaments stiffen. When the cartilage wears down, the bones may rub together causing pain (Fig. 1). The SI joint is a synovial joint filled with fluid. This type of joint has free nerve endings that can cause chronic pain if the joint degenerates or does not move properly.
Sacroiliac joint pain ranges from mild to severe depending on the extent and cause of injury. Acute SI joint pain occurs suddenly and usually heals within several days to weeks. Chronic SI joint pain persists for more than three months; it may be felt all the time or worsen with certain activities.
Other terms for SI joint pain include: SI joint dysfunction, SI joint syndrome, SI joint strain and SI joint inflammation.
What are the symptoms?
The signs and symptoms of SI pain start in the lower back and buttock, and may radiate to the lower hip, groin or upper thigh. While the pain is usually one sided, it can occur on both sides. Patients may also experience numbness or tingling in the leg or a feeling of weakness in the leg.
Symptoms may worsen with sitting, standing, sleeping, walking or climbing stairs. Often the SI joint is painful sitting or sleeping on the affected side. Some people have difficulty riding in a car or standing, sitting or walking too long. Pain can be worse with transitional movements (going from sit to stand), standing on one leg or climbing stairs.
What are the causes?
The SI joint can become painful when the ligaments become too loose or too tight. This can occur as the result of a fall, work injury, car accident, pregnancy and childbirth, or hip/spine surgery (laminectomy, lumbar fusion).
Sacroiliac joint pain can occur when movement in the pelvis is not the same on both sides. Uneven movement may occur when one leg is longer or weaker than the other, or with arthritis in the hip or knee problems. Autoimmune diseases, such as ankylosingspondyloarthropathy, and biomechanical conditions, such as wearing a walking boot following foot/ankle surgery or non-supportive footwear, can lead to degenerative sacroiliitis.
How is a diagnosis made?
A medical exam will help determine whether the SI joint is the source of your pain. Evaluation includes a medical history and physical exam. Your physician will consider all the information you provided, including any history of injury, location of your pain, and problems standing or sleeping.
There are specific tests to determine whether the SI joint is the source of pain. You may be asked to stand or move in different positions and point to where you feel pain. Your doctor may manipulate your joints or feel for tenderness over your SI joint.
Imaging studies, such as X-ray, CT, or MRI, may be ordered to help in the diagnosis and to check for other spine and hip related problems.
A diagnostic SI joint injection may be performed to confirm the cause of pain. The SI joint is injected with a local anesthetic and corticosteroid medication. The injection is given using X-ray fluoroscopy to ensure accurate needle placement in the SI joint. Your pain level is evaluated before and 20-30 minutes after injection, and monitored over the next week. Sacroiliac joint involvement is confirmed if your pain level decreases by more than 75%. If your pain level does not change after the injection, it is unlikely that the SI joint is the cause of your low back pain.
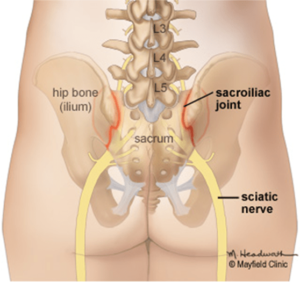
Fig. 1. The sacroiliac joints connect the base of the spine (sacrum) to the hip bones (ilium).
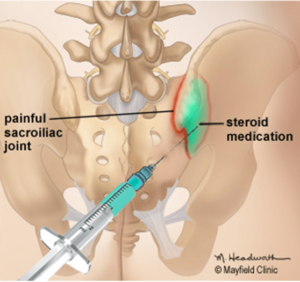
Figure 2. A needle is gently guided into the sacroiliac joint using x-ray fluoroscopy. An anesthetic and corticosteroid mixture (green) is injected into the inflamed joint.
What treatments are available?
Nonsurgical Treatments:
Physical therapy, chiropractic manipulation, and stretching exercises help many patients. Some patients may require oral anti-inflammatory medications or topical patches, creams, salves or mechanical bracing.
Joint Injections:
Steroids can reduce the swelling and inflammation of the nerves. Joint injections are a minimally invasive procedure that involves an injection of a corticosteroid and an analgesic-numbing agent into the painful joint (Fig. 2). While the results tend to be temporary, if the injections are helpful they can be repeated up to three times a year.
Nerve Ablations:
Injections into joints or nerves are sometimes called “blocks.” Successful SI joint injections may indicate that you could benefit from radiofrequency ablation – a procedure that uses an electrical current to destroy the nerve fibers carrying pain signals in the joint.
Surgery:
If nonsurgical treatments and joint injections do not provide pain relief, your physician may recommend minimally invasive SI joint fusion surgery. Through a small incision, the surgeon places titanium (metal) implants and bone graft material to stabilize the joint and promote bone growth. The surgery takes about an hour. The patient may go home the same day or following day. For several weeks after surgery, the patient cannot bear full weight on the operated side and must use crutches for support.
Recovery & Prevention
A positive attitude, regular activity, and a prompt return to work are all very important elements of recovery. If regular job duties cannot be performed initially, modified (light or restricted) duty may be prescribed for a limited time.
Prevention is key to avoiding recurrence:
- Good posture during sitting, standing, moving, and sleeping
- Regular exercise with stretching /strengthening
- An ergonomic work area
- Good nutrition, healthy weight, lean body mass
- Stress management and relaxation techniques
- No smoking
Sources & links
If you have questions, contact Mayfield Brain & Spine at 800-325-7787 or 513-221-1100.



